Wisdom Molar Pain
What is causing it, how to manage it, and when professional treatment is the only answer
Pain at the very back of the jaw — in the area of the wisdom teeth and the molars behind them — is one of the most common dental complaints, and one of the most frequently misunderstood. Patients often describe it as generalised aching in the back of their mouth, sometimes radiating to the ear or jaw, sometimes focused on a specific tooth, sometimes impossible to localise precisely.
Wisdom molar pain is a broad term that covers a range of clinical presentations — from the normal, temporary aching of a wisdom tooth pushing through gum tissue, to an acute infection that needs professional treatment the same day. The key to managing it well is understanding which of these you are dealing with.
At Lateral Dental Clinic in Sheffield, led by Dr Matthew Stephens GDC No. 263989 and Dr Anupa Stephens GDC No. 264031, we assess and treat problems in the wisdom tooth and molar region regularly. This guide covers the full clinical picture: the anatomy behind why this region is so prone to problems, the specific causes of pain, what each one requires, and how to tell the difference between something you can manage at home and something that needs professional assessment today.
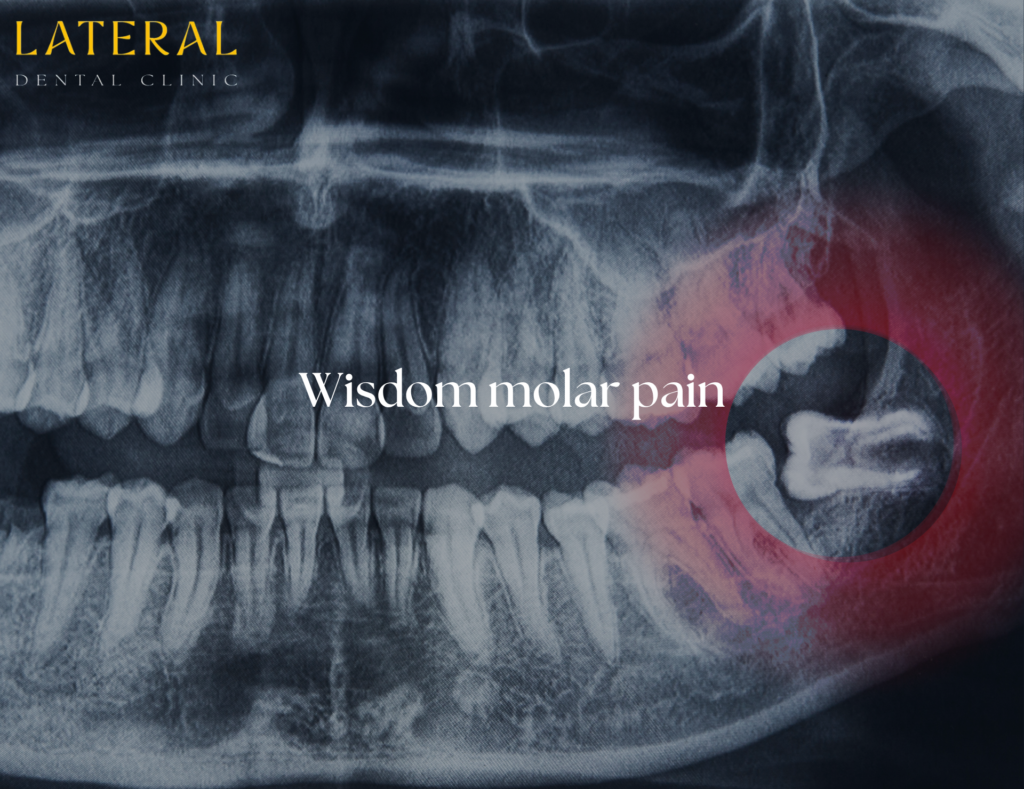
The anatomy of the back of the mouth: why this region causes so many problems
The back of the mouth — the region occupied by the second and third molars — is clinically challenging for several anatomical reasons that directly explain why wisdom molar pain is so common.
The third molar’s late arrival
The wisdom teeth (third molars) are the last teeth to develop and erupt, typically between the ages of 17 and 25, though eruption into the thirties is not unusual. By the time they attempt to emerge, every other permanent tooth is established, the jaw has finished growing, and there is frequently insufficient space to accommodate them. This is the foundational reason why wisdom teeth cause problems disproportionate to their size.
Restricted access for cleaning
Even wisdom teeth that erupt fully and in a reasonable position sit at the very back of the mouth, where toothbrush access is awkward at best. The second molar directly in front of the wisdom tooth is the tooth most commonly affected by decay and gum problems related to this access issue — the contact area between the wisdom tooth and the second molar traps plaque and food in an area that most brushing technique misses entirely.
The inferior alveolar nerve
In the lower jaw, the roots of the lower wisdom teeth frequently sit in close proximity to the inferior alveolar nerve — the nerve that provides sensation to the lower lip, chin and teeth on that side. This proximity means that pain in the wisdom tooth region can radiate along the nerve pathway and be felt in the teeth in front of it, in the jaw, in the ear, and sometimes down the neck — creating a pain pattern that is far larger than the source.
What causes wisdom molar pain?
1. Eruption pressure
The most basic cause of wisdom molar pain is simply the physical process of a tooth pushing through the bone and gum tissue. This is the most benign cause and the most common, but it can still produce genuine, sometimes significant discomfort.
What it feels like: A dull, aching pressure at the back of the jaw, often with mild swelling of the overlying gum. The pain comes and goes as the tooth moves through in stages — it may be present for a few days, ease for several weeks, then return when the tooth moves again.
Duration: Intermittent episodes over months, sometimes longer. Each episode typically lasts three to seven days before settling.
What helps: Over-the-counter pain relief — ibuprofen being the most effective for its anti-inflammatory as well as analgesic action — warm salt water rinses, and keeping the head elevated during sleep to reduce vascular pressure. The discomfort resolves between active eruption phases without any treatment.
When to worry: Eruption pain that is progressing rather than easing, that is severe rather than moderate, or that is accompanied by swelling or a bad taste suggests that something beyond straightforward eruption is happening.
2. Pericoronitis
Pericoronitis is an infection of the gum tissue surrounding a partially erupted wisdom tooth, and it is one of the most clinically significant causes of wisdom molar pain. When a wisdom tooth has partially broken through the gum, the overlying flap of tissue creates a pocket that traps bacteria, plaque and food debris in an environment that is essentially impossible to keep clean.
What it feels like:
- Throbbing, persistent pain at the back of the jaw — typically more severe than eruption discomfort
- Localised swelling of the gum tissue around the wisdom tooth
- A bad taste or unpleasant smell from the infected area
- Tenderness spreading towards the ear, jaw and throat on the affected side
- Difficulty opening the mouth fully in more severe presentations (trismus)
- Swollen lymph nodes beneath the jaw or in the neck
What makes it different from eruption pain: The character of the pain. Eruption pain tends to be a background ache that eases and returns. Pericoronitis pain is typically more severe, more persistent, often accompanied by the soft tissue signs described above, and does not settle on its own without intervention.
Treatment: Mild pericoronitis can sometimes be managed with professional irrigation of the infected pocket, improved oral hygiene around the area, and short-term pain relief. More significant infections require antibiotics alongside local treatment. Crucially: pericoronitis that has occurred once from the same wisdom tooth is likely to recur. The anatomy that makes the pocket susceptible to infection does not change unless the tooth is extracted or the gum flap removed. Recurrent pericoronitis from the same tooth is one of the clearest clinical indications for wisdom tooth extraction.
3. Impacted wisdom tooth pressing against the second molar
An impacted wisdom tooth — one that cannot erupt normally because it is blocked by the adjacent second molar, the jawbone, or the tooth’s own angulation — creates a pattern of wisdom molar pain that is different from eruption pain or pericoronitis. Because the wisdom tooth is applying direct pressure against the roots of the second molar, the pain is often felt in the second molar itself rather than, or in addition to, the wisdom tooth.
The clinical problem: The second molar is a tooth that should be perfectly healthy. When a mesially impacted wisdom tooth (angled towards the front of the mouth) presses against its roots, it can cause:
- Resorption of the second molar root surface — the second molar’s root is being physically damaged by the pressure from the wisdom tooth
- Decay on the contact surface between the two teeth — the impacted wisdom tooth creates a cleaning trap that allows decay to progress on the second molar
- Periodontitis (gum disease) in the pocket between the two teeth — with associated bone loss
These complications are largely painless until they are advanced, which is one of the most compelling reasons for regular dental check-ups that include X-rays of the wisdom teeth and the teeth in front of them.
When pain does develop from an impacted wisdom tooth pressing against the second molar, it tends to be a deep, constant aching pressure rather than the more acute, fluctuating pain of pericoronitis. Biting down may worsen it.
Treatment: The definitive treatment for a significantly impacted wisdom tooth causing pressure symptoms or damage to the second molar is extraction. The severity of any existing damage to the second molar determines whether it can be managed conservatively — a large cavity caused by the impaction may require root canal treatment and a dental crown, or in more extreme cases where the root has been extensively resorbed, extraction of the second molar may also be necessary.
This is precisely why early identification of impacted wisdom teeth matters. Caught before significant damage occurs, the management is simpler and the outcome for the second molar better.
4. Decay in the wisdom tooth or the adjacent second molar
The cleaning difficulty that comes with wisdom teeth makes the molar region the most cavity-prone area of the adult mouth. Decay can develop in the wisdom tooth itself, in the second molar, or in both simultaneously — and the pain patterns can overlap, making it difficult to identify the specific tooth responsible without clinical examination and X-rays.
Decay-related pain presentation:
- Early decay: Often entirely painless, identified only on X-ray
- Dentine-level decay: Sensitivity to sweet foods, cold and sometimes heat; usually brief and responsive to the stimulus
- Deep decay approaching the pulp: More prolonged sensitivity that lingers after the stimulus has been removed
- Pulpal involvement: Spontaneous, constant aching that is often described as throbbing and worst at night — indistinguishable in character from other pulpal pain
Treatment options: Where decay is caught early in the wisdom tooth, a filling may be possible if the tooth is in a reasonable position and can be cleaned effectively long-term. Where decay is extensive, where the tooth is poorly positioned, or where pulpal involvement has occurred, extraction is often the more pragmatic clinical choice. For the second molar — a tooth with significantly more functional importance — the effort to preserve it is greater, and root canal treatment followed by a protective dental crown is the standard approach where decay has reached the nerve.
5. Gum disease in the molar region
The same access problems that make the molar region prone to decay also make it the area of the mouth where gum disease most commonly becomes established and progresses to its more destructive stages. Periodontitis — the advanced form of gum disease involving bone destruction — often affects the lower wisdom teeth and second molar region disproportionately.
What it causes: Gum disease in the molar region tends to cause a dull, generalised aching and sensitivity rather than sharp tooth pain, alongside bleeding gums, visible gum recession, and a persistent bad taste. The pain tends to be less acute than pulpal or abscess pain but more persistent.
Why it matters beyond the pain: The bone loss associated with periodontitis in the wisdom tooth region can undermine the second molar as well. Advanced bone loss at the distal aspect (back surface) of the second molar — caused by the wisdom tooth’s position making that area impossible to clean — can make a previously healthy second molar require extraction.
This is managed through general dental treatment including professional deep cleaning (root surface debridement), improved home care, and in some cases extraction of the wisdom tooth to make the area cleanable.
6. Wisdom molar abscess
An abscess in the wisdom molar region — from either a dying pulp in a deeply decayed wisdom tooth or an acute periodontal abscess from gum disease — produces the most severe category of wisdom molar pain.
Presentation:
- Severe, throbbing, constant pain that does not respond adequately to over-the-counter analgesics
- Swelling of the gum tissue alongside the tooth, or visible swelling of the cheek and lower face
- A bad taste or discharge suggesting pus drainage
- Fever and feeling unwell in more advanced cases
- Difficulty opening the mouth or swallowing
This presentation requires same-day dental assessment. An abscess will not resolve without professional treatment — antibiotics control the spread of infection but do not drain the pus or eliminate the source. The definitive treatment depends on the cause and the condition of the tooth involved.
Wisdom molar pain vs other molar pain: how to tell the difference
One of the most clinically confusing aspects of pain in the back of the mouth is distinguishing between wisdom molar pain and pain originating from one of the other molars. Some pointers:
Pain most likely from the wisdom tooth:
- Located specifically at the very back of the jaw, beyond the last erupted tooth
- Accompanied by swelling or redness of the gum tissue at the back of the mouth
- Came on during a period when the wisdom tooth has been actively erupting
- Associated with difficulty opening the mouth fully
Pain most likely from the second molar or first molar:
- More precisely localised to a specific tooth that can be identified on tapping
- Associated with recent dental work, a large old filling, or visible decay
- Responds sharply to cold or hot stimulation and lingers
- The wisdom tooth area appears and feels normal
Why it sometimes cannot be distinguished without examination and X-rays:
- Referred pain along the inferior alveolar nerve means wisdom tooth problems are regularly felt in the teeth anterior to the wisdom tooth
- Decay on the distal surface of the second molar caused by an impacted wisdom tooth feels identical to primary second molar decay
- Both conditions can coexist simultaneously
A proper clinical assessment — examination with percussion and vitality testing, combined with diagnostic X-rays — is the only way to reliably identify the source.
When is wisdom molar pain a dental emergency?
The following symptoms mean you should seek dental assessment today rather than booking a routine appointment:
- Severe, constant pain that is not controlled by maximum doses of ibuprofen and paracetamol
- Swelling of the face, cheek or neck
- Difficulty opening the mouth or swallowing
- Fever alongside dental pain
- A bad taste or discharge in the mouth
- Spreading pain or swelling that appeared rapidly over the course of hours
At Lateral Dental Clinic in Sheffield, we provide emergency dental appointments for exactly these situations. Dr Matthew Stephens and Dr Anupa Stephens and the team will assess you thoroughly, take the X-rays needed, and get you on the right clinical path the same day.
Managing wisdom molar pain at home
While arranging an appointment, the following measures help manage discomfort:
- Ibuprofen is the most effective OTC option — it addresses both pain and the inflammatory component. 400mg with food, up to three times daily at intervals of at least four to six hours. Combining with paracetamol (taken at separate, recommended doses) provides enhanced relief.
- Warm salt water rinses — half a teaspoon of table salt in a glass of warm water, rinsed gently two to three times a day — reduce bacterial load around the affected area, soothe inflamed gum tissue, and help keep any partially erupted tooth area clean.
- Head elevation — sleeping propped up reduces the vascular pressure that worsens overnight throbbing.
- Cold compress — applied to the outside of the cheek for 15 to 20 minutes at a time to reduce swelling and dull pain signals.
These measures reduce symptoms. They do not treat the underlying cause.
What if you are anxious about treatment?
Anxiety about dental treatment is one of the most common reasons patients delay having wisdom molar pain properly assessed — and unfortunately, the delay typically allows the clinical situation to deteriorate.
At Lateral Dental Clinic, we offer conscious dental sedation for patients who find dental treatment difficult. This allows clinical examination, X-rays and treatment — including wisdom tooth extractions where needed — to be carried out while you remain deeply relaxed, with little to no memory of the appointment afterwards. Many patients who had been putting off treatment for months or years because of anxiety describe their sedation appointment as genuinely transformative.
If dental anxiety has been keeping you from addressing wisdom molar pain, please mention it when you book. We will make sure the appointment is planned around your needs.
The bottom line
Wisdom molar pain covers a spectrum from manageable eruption discomfort that settles with time and home care, to acute infections and impaction-related damage that require prompt professional treatment. The key clinical questions are: is the pain fluctuating or constant? Is it accompanied by swelling, fever or spreading symptoms? Has it been present for more than a week without improvement? Is this the second or third time this has happened from the same area?
If the answer to any of those is yes, professional assessment is the appropriate response — not continued home management.
At Lateral Dental Clinic in Sheffield, Dr Matthew Stephens GDC No. 263989 and Dr Anupa Stephens GDC No. 264031 offer thorough assessments for wisdom molar pain — from examination and X-rays to whatever treatment the clinical picture requires, including root canal treatment for affected molars, crowns to protect restored teeth, and sedation for patients who need it.
Disclaimer
The information in this article is intended for general guidance only and does not constitute personalised dental or medical advice. If you are experiencing severe pain, swelling, fever or difficulty swallowing alongside wisdom molar pain, please seek emergency dental care promptly.
Lateral Dental Clinic is a private dental practice in Sheffield, led by Dr Matthew Stephens GDC No. 263989 and Dr Anupa Stephens GDC No. 264031. We offer general dentistry, root canal treatment, dental crowns, dental sedation, Invisalign, composite bonding, porcelain veneers, teeth whitening and smile makeovers.
Questions our patients ask about wisdom molar pain
It is often genuinely difficult to distinguish without clinical examination and X-rays, and this is one of the most common clinical puzzles in the wisdom molar region. Wisdom tooth pain tends to be felt at the very back of the jaw and is often accompanied by gum swelling behind the last visible molar. Second molar pain from impaction-related decay can feel identical to primary molar decay. A proper clinical assessment at Lateral Dental Clinic — including percussion testing and diagnostic X-rays — is the only reliable way to identify the correct source and plan the appropriate treatment.
It depends on the cause. Normal eruption discomfort will ease between active movement phases and may settle eventually once the tooth has fully erupted. Pain from pericoronitis, impaction, decay or abscess does not reliably resolve without professional treatment — it typically persists or worsens. If pain has been present for more than a week, has recurred after a previous episode, or is accompanied by swelling or fever, it needs clinical assessment rather than continued home management.
Not necessarily, and this is an important clinical point. When severe dental pain stops suddenly without treatment, it can mean the nerve has died — the pulp tissue has become necrotic, removing the source of the pain signal. The infection does not stop, however: it continues to progress through the root apex into the surrounding bone, often developing into a dental abscess. A tooth that stops hurting suddenly should be assessed by a dentist promptly rather than assumed to have resolved. Book an appointment with the Lateral Dental Clinic team.
Yes — this is one of the most significant clinical risks of an unmonitored impacted wisdom tooth. A mesially impacted lower wisdom tooth pressing against the second molar can cause root resorption, decay on the contact surface and bone loss from periodontitis — all of which can compromise or in severe cases destroy the second molar. This damage occurs largely without pain until it is advanced, which is why regular X-rays of the wisdom tooth region are part of routine dental care at Lateral Dental Clinic. Where significant damage to the second molar has already occurred, root canal treatment and a dental crown are the options for preserving it.
At Lateral Dental Clinic, conscious dental sedation is available for patients who find dental treatment difficult. Sedation is suitable for assessments, X-rays, extractions and all associated procedures — you remain comfortable and relaxed throughout, with little to no memory of the appointment. Dental anxiety is very common and completely understandable, and it should never be the reason wisdom molar pain goes unassessed and untreated. Please let us know when booking and we will plan your appointment accordingly.